Sorry to hear of this, Terry. Some things happen due to genetic predisposition and not anything that you may have done or not done. I wish you the best of outcomes.
when I wrote,“I was just curious…” I meant that in the past tense. there was no need to continue discussing something u didn’t want to in the first place! 
I’m sorry to hear about this Terry. I hope the results of the future tests are in the best ranges possible.
Thanks for sharing your knowledge about coronary artery disease. I’m learning a lot from posts on this thread.
While I wouldn’t wish this on you or anyone, I admire you for sharing your experiences so that we can all learn. It’s also comforting to read about all the support people on here are offering you. I hope you realize the impact you had on others in those posts 
Thank you so much for this. Your comment and several others have touched me at a deep and sensitive level. I have been teary more than once!
When Manny Hernandez (@askmanny) founded TuDiabetes more than ten years ago, his founding focus was that no one with diabetes every feel that they’re alone. While I’ve always acknowledged the emotional wisdom of that sentiment, it’s true meaning has never been felt more strongly by me than now!
We have an amazing power to help each other. We should stay focused on that and less on some of the more contentious issues we talk about. And I have been just as guilty of that as any member. I know conflict can yield learning but I think we interact best when we try to remain civil and as kind as possible.
I thank-you all from the bottom of my dysfunctional heart!
Norm’s empathy always amazes me. I am so lucky he’s my constant companion.
Sandy, I appreciate your kind and generous offer. Your medical background combined with living with T1D provides a view not many medical providers share. Those of us who live with diabetes 24/7 accumulate a depth of knowledge and understanding of diabetes that the credentialed class often fail to see.
That’s not meant as hurtful criticism, just an acknowledgement of human nature and reality. I’m grateful to live at a time in history where I have access to people who devote their lives to the practice of medicine.
As I move through this process, I may have a question or three for you! Thank-you, that means a lot to me.
Norm’s got some pretty sweet freckles on his nose. I’m glad you have each other.
Thanks, @Sprocket1. From the looks of your avatar, you enjoy some canine companionship, too!
Thank you for sharing. All this is on my mind daily plus kidney disease. The harder I try to watch it the more my sugars go crazy. Love reading your posts they are so encouraging and full of information. I don’t have a support system or a good endo. But I read a lot You got this covered. I do take Lipitor and my LDL is at 68. I was told by my cardiologist that it would help toward getting heart disease. My husband does and has already had open heart surgery at 56 and 3 stents so I have asked over and over what to do to help me. I’m lucky I don’t have a family history of any of that or diabetes but I got the diabetes which they say was from stress. All I know is I want to be around another 20 plus years to see my grandkids grow up. One question how long you been a diabetic? Thank you for sharing. And you are the first person I look for in here.
Kathy, thanks so much for your note and encouragement. I’ve been lucky with my kidneys. Going through what I am now, I can really appreciate what dealing with kidney disease must mean for you. We have to adjust, take care of business, and do the best we can.
Next January will mark 35 years with diabetes. I was 30 at the time. I count my blessings that my childhood and teenage years passed with a healthy glucose metabolism. This is a tough disease.
Take care! Do something nice for yourself today.
A stress echocardiogram test was performed on me this morning. It involved laying on a bed and peddling a recumbent bicycle to get my heart rate up to 85% of my calculated maximum heart rate. I was hooked up to several heart sensors stuck to my chest. I had a blood pressure cuff on during the entire test and it periodically inflated to record my blood pressure. I also had an IV in my arm to provide contrast for the ultra-sound images.
The main part of the test was using an ultra-sound device to take images of my heart, both at rest and under physical exertion. The test was uneventful and I finished before the time they allotted to my procedure.
Norm was well-behaved on the floor, not too far away. I kept my CGM receiver, iPhone with my Loop dashboard, and some glucose tabs all within easy reach. I don’t think either the nurse or technician has come into contact with a patient who prefers not to lose sight of real-time BG readings.
My glucose, even with the sweat-breaking 8-12 minutes of work did not break from a solid 83 (4.6) line. It’s spooky how well behaved my BG lines have been lately. It’s been two weeks since I reduced my daily carbs down to Bernstein levels. I now wish that the BG fight was the only one I needed to engage. Oh, well! Play the hand you’re dealt.
I have an appointment with a talk therapist next week. I continue to try and identify all the pieces of this puzzle that I need to address.
Did they give you any info on if you had any segment depressions or elevations?
The nurse and the technician were pretty tight-lipped with what they were seeing beyond giving me status updates on reaching the target heart rate. I asked what my oxygenation was and she said, 95%. I’ll have to wait for my doctor to give me the results. I am going to ask for all the raw data I can get. I hope I don’t get turned down with any of the data.
What is a segment depression or elevation?
The shape of the ECG can give an indication of what is happening with your heart.
It’s obviously not something somebody can read without training, but I was wondering if they told you anything.
If you have a depression or an elevation that looks different when your heart starts to become under stress, it can indicate if it is not getting enough oxygen or if there or arrhythmias or things like that.
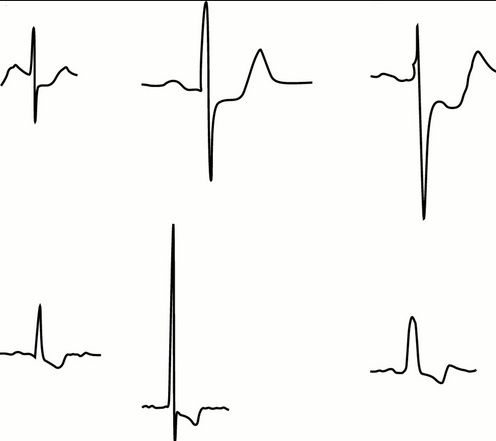
Here are some different ECG patterns. The different shapes are things they look at. And also which of the leads they came from of the 12 leads they had hooked on your body (anterior, inferior, lateral, etc.).
So sorry to hear this @Terry4, but it sounds like in the time before the shock of the diagnosis and deciding to write about it you’ve started to gather strength in confronting and dealing with it. You’ve been such a positive and informative presence here that I feel much confidence that you’ll manage this as well.
I have a whole new set of facts to learn. While I certainly don’t expect any mastery level of knowledge to occur, I hope to learn as much as possible so that I can reasonably assess, from a patient’s perspective. After I asked you the question, I went to Google and found some understandable info. I appreciate your obviously informed comments on this topic!
Thank-you, @DrBB. My goal is to do the best I can. I want to be as informed as possible and I don’t want to go along traditional medicines’s path unless it makes sense for me.
I appreciate the service you and the other admins so generously give to this community. Keep up the good work!
@Terry4, t does indeed take courage to face this, and then to write about it here. I can identify with your post. I had a bad fall in 2012 and injured my head. Subdural hematoma was diagnosed, and holes were drilled in my skull to drain out the blood that was pressing against my brain.
I was told by my doctor that I was very fortunate to live through the accident, and the operation.
We never know how a serious situation will turn out. You may be alive and still productive for many more years. I hope that will ring true for you!!
Although I had a near fatal cardiac arrest close to nine years ago, I have not been diagnosed with any coronary disease. I attribute that in large part to a book I read half a century ago, when I was a teenager, called, I believe, You are what you eat.
So my whole life I’ve not eaten red meat (beef), I’ve made sure to get my six or seven servings of veggies or fruit a day, I’ve used liberal amounts of olive oil or Canola oil, eaten fish three times a week (sometimes a can of sardines at lunchtime, sometimes a salmon steak for dinner and avoided sugar like the plague. According to my cardiologist a recent checkup indicated no hardening or clogging of any of my arteries. In fact, he said I am probably good to go until I’m 90. Which to me shows the incredible effect that healthy choices of what you eat are the key to good health and longevity. (Ah yes, I do have my diabetes type 2 but can’t blame that on lifestyle. I have an inherited genetic ailment called hereditary hemochromatosis which results in a buildup of iron in internal organs and in my case zapped my panchreas before I was diagnosed at age 50 and could be treated with regular blood lettings.)
Just an opinion here from whole-food plant based diet guy who follows Dr. Gregor, among others.
One item at a time. I’m picking limited items you mentioned.
The way to optimize gut health is with a high fiber plant-based diet devoid of animal products otherwise called vegan. Greger and others refer to it’s ability to reverse CAD, and particularly the atheroschelotic process. At debate is how much a reversal and that depends on how perfect the diet is. Even a 10% reversal is worth it, IMHO.
NOTE THAT I AM NOT RECOMMENDING ANYTHING BUT ONLY GIVING INFORMATION.
The’re an rx omega 3 that’s popular with no EPA or DHA (since they can form end products that include araodonic acid) but merely pure omega 3. It is a script called VASCEPA that best fits that criteria, taken as four one g caps per day typically, and not cheap. The official line is to lower your elevated trigs. Vegans as a group have very low omega 3 --which is not good. In fact their (or our, insofar as I am one too) have the worst (lowest) ratio of w3 to w6. Anyway, recall that lower w6 is part of the “good” plan since it’s in most everything you eat already and not helpful to supplement that beyond the normal reference range. You know your doc can order the levels in a lab that will report serum w3. w6. and w3/w6. w6 forms a pro-inflammatory metabolite unlike w-3.
Here’s the story on DHA and EPA, which is why they are questionable to supplement.
DHA has little effect on cellular inflammation, whereas EPA reduces inflammation since it is an inhibitor of delta-5-desaturase (D5D). D5D produces AA. More EPA in the diet suggests that you produce less AA. DHA does not inhibit D5D. DHA increases LDLc, unlike EPA.
Oddly there’s a better metric than w3/w6 according to some literature. If it’s not better than it may be more predictive of events. It’s called “omega 3 index” and curiously is the sum of DHA and EPA expressed as a percentage of total phospholipid fatty acids. The prevailing thought is that w-3 index is more accurate prediction of CV events than either w-6/w-3 ratio or the EPA or DHA levels. Association between w-3 index and cardiovascular events is based on repeated findings such as reported by Albert et al. NEJM. 2002;346:1113. It’s easy to google.
I’ve been on the K2 story and know there a vast literature. I think but do not know if the latest official line is that there is inadequate evidence to demonstrate blah, blah, blah. . . Who know? For what it’s worth, I take it only a certain one with the right subcomponent. But what I take has no bearing on anybody else.
I prefer to get nutrients from actual real food, not supplements. And many supplements in the absences of any nutritional deficiency can increase risks of terrible events like lung or prostate cancer. It’s off topic to give that list here. Now I realize that a lot of people don’t know that and will choke upon reading that so let me just say talk to your doc if one wishes to debate it. People just love their supplements is proven by the however-many billions of dollars spent on it, much of which is on the scale somewhere of nonsense to inadequate justification, according to experts. You can form your own opinion.
Experts say a lot of people are low in Vit D. It’s easy enough to find out with a 1,25-dihydroxy, serum lab called calcitriol. That’s the active form that regulates Ca and phos in kidneys and elsewhere. The 25-hydroxy version called calcifidiol is still useful to know too. The two labs can be ordered simultaneously.
There’s a lot more to everything mentioned as well as the practice of medicine which is why you let your doctor do that. He or she will now, for instance, and picking one example of K2 and Ca metabolism in the context of some particular disease, like osteoporosis that some people have, know how and when (if at all) to order a lab for osteocalcin (OC) (vs creatinine kinase). OC is a bone turnover marker that relates to K2 and cardo health. You might not have osteoporosis. It is a common example of a possibility. I mention it as an example to explain clinical thinking in the context of our S/S and lab findings. For instance, a common use is OC increase correlates in your doc’s mind as a marker for effectiveness of BMD anabolic med in Tx for osteoporosis according to Szulc et al: ucOC inversely correlates w/ BMD Knapen et. al. Also Vergnaud et al: serum ucOC predicts hip fracture. And Luukinen et al and Szulc et al: high ucOC//6-fold increase fracture risk. Don’t trust me, look it up. Oh, the little uc in ucOC stands for uncarboxylated. I gave one of a hundred examples of things the doc will take into account for some but not for others who it could be entirely irrelevant.
Finally, on an EKG, is a QRS narrow or wide? That’s my first of several easy to spot things to look at. Narrow is good because by definition it means to rule out VT, VF, or hearth block – the three serious and potentially fatal issues where people drop dead.
Provided one has a normal or almost-normal EKG, meaning nothing obvious like WPW, BBB, this or that details of note like inverted t waves, delta waves, or Brugada which could be interesting, if there’s no wild brady or tachy, then mostly everything else is managable by ordinary and simple means (med, diet, lifestyle) if and only if it’s in the absence of family history sudden death and provided one doesn’t have S/S namely syncope or palpitations and provided we don’t smoke. If one has syncope then that’s generally a bad predictor. It’s not that complicated considering how much they get paid on average.
But sure, as others said, any cardiologist can send you for a catheterization (including renals too while there may be useful so ask) to determine your ejection fraction (EF), and a coronary CT is different but very common and useful when cQRS is long. The little c mean corrected. Either way without all that, management is not that complicated. So a cardiac W/u is routine eval. But is also urgent only in the context of you history and S/S. One hopes that an EF is above 50%. The big secret is a lot your EKG doesn’t mean much or correspond directly to outcomes so don’t worry to much about minutia is a legitimate opinion (unless one has syncope or other real dangerous sequelae and then dig deaper to reveal nuanced information.) This is why you let your doc do his job.
Lifestyle, lifestyle, lifestyle. . . Best wishes
one more thing. . .
They didn’t have any leads hooked to your body. “leads” means what’s the printed 12 parts on the EKG strip. What was hooked to your body was electrodes not leads. And there were 10 not 12 of them to get the 12 leads on the strip. And it’s actually 13 leads shown on the strip since it shows 6 seconds of II at the bottom of the strip. Count them and you 'll see.

